The median savings account balance in the U.S. is $4,500. While that is enough to cover rent it may not be enough to also cover the cost of medications. 87% of Americans say the affordability of healthcare is at least a moderately big problem in their day to day lives. Patient adherence to their prescriptions is largely driven by drug affordability, specifically the out of pocket cost of medications. Helping patients lead healthier, more proactive lives is the purview of every healthcare organization, especially those working on drug affordability.
A Top of Mind Issue
Patients need help paying for their medications. If you’ve interacted with the healthcare system at all, you know that drugs have become expensive, oftentimes too expensive. Drug affordability is top of mind for everyone: nationwide out of pocket costs for prescription medicines was $79 billion in 2021, up from $74 billion in 2015. The average price for newly marketed prescription drugs in the US has grown by 20% annually for the past 13 years and shows no signs of slowing down.
Unfortunately, the concept of drug affordability is not just about putting money back in patient’s wallets. There’s a dangerous behavioral byproduct. Expensive medications also drive patient nonadherence and poorer health outcomes, increasing the overall cost of care.
The Impact of Affordability on Adherence
This is not a small problem.
-
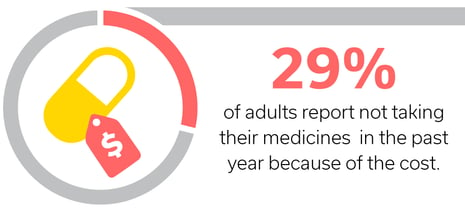
About three in ten of all adults report not taking their medicines as prescribed at some point in the past year because of the cost
-
More than 2 of every 3 Americans abandon their prescription medication when their out-of-pocket costs reach $250 per dose.

-
Six therapy areas account for 42% of total high-cost prescriptions (>$125): diabetes, obesity, asthma, COPD, stroke, and HIV drugs.
Many researchers have documented the nature of non-adherence when patients can’t afford their medications. One in five will take an over-the-counter drug instead (18%). One in 10 (12%) will self-ration their doses or skip a dose entirely. Unsurprisingly, about a third of those who report not taking their medicines say their condition got worse as a result, nearly 4x higher than the 8% of patients who report their condition got worse after staying compliant to a prescribed therapy regimen.
While there are often programs and opportunities available to help patients pay for their prescriptions, patients aren’t always aware of their options. Understanding that cost is the primary gating factor to initiating and staying on medication, how can pharmaceutical manufacturers and Access teams assist patients?
New Awareness Opportunities Start at Enrollment
Up to 50% of medications are not even started by Medicare Part D recipients if the patient does not receive assistance in paying for the medication. However, only 65% of patients and caregivers in a national survey reported that they have successfully enrolled in a copay assistance program.
Access teams have a massive opportunity to increase awareness and patient mindshare about their savings and affordability programs. Savings programs play a crucial role in initiating and ultimately adhering to medication. We know that these programs are highly effective for patients that enroll, as 6 in 10 enrolled patients say they would have extreme difficulty affording treatments and medications without copay assistance.
Why is uptake of copay and financial assistance programs relatively low, even though they can offer compelling benefits for patients? Enrollment into savings programs is often clunky, requiring and locating an obscure enrollment PDF form buried on a therapy website, or creating an account on yet another portal.
For example, if a patient had Crohn’s Disease, and was prescribed Humira, they would need to do the following to enroll in the Humira savings program:
-
Navigate to https://www.humira.com/crohns
-
Navigate to ‘Starting Humira’ amongst the four other options that are presented at the top of the homepage
-
Click on ‘Save on Humira’ amongst the eight other options
-
Sign up for ‘Humira Complete’
-
Select the right condition, which AbbVie already knows from the website is Crohn’s Disease
-
Select ‘I am prescribed Humira’
-
Fill out the prescription date, First Name, Last Name, Email Address, and then click the “Sign Up” button
-
Fill out an insurance form, provide and address (again)
-
Tell the Nurse Ambassador the preferred time to be called, and provide a phone number
-
Enter date of birth, zip code, gender
-
Create a strong password — a mix of upper/lower case, numbers, symbols, 10+ characters
-
Wait for call back from Nurse Ambassador to complete enrollment
-
Upon receiving the call days later the time comes to remember the Humana username and password in order to re-enter the portal as the case is processed
This complex, multi-step process creates significant friction for patients, and can disproportionately impact patients who are less digitally- or health-literate. To even the playing field and ensure access, manufacturers need to introduce patients to affordability programs in a streamlined, engaging manner at the right health literacy level, as close to the prescription moment as possible.
A Reimagined Approach to Increase Affordability Program Awareness
To increase awareness of affordability programs, Access teams must meet patients in their preferred mobile engagement channels. Today, 86% of adults carry advanced smartphones and most use them extensively as part of their daily lives. While mobile apps bring additional engagement complexity, other mobile engagement channels are maturing and proving to be very effective in helping patients navigate healthcare.
While relatively few patients will visit a therapy brand.com website, and less than 19% will pick up a call from a random number, 81% of patients want to interact with their healthcare service providers via mobile messaging. Conversational messaging is effective because it is simple to use and delivers results.
Engaging patients via mobile messaging is a win-win for manufacturers: 97% of text messages are opened in 3 minutes or less, and Conversational AI technology has matured sufficiently to augment affordability conversations that case managers or navigation teams typically manage (e.g. how to enroll, eligibility criteria, impact on copays). What would this look like in practice?
By leveraging automated conversational engagement, Access teams can ensure that every patient they are in contact with receives personalized education and assistance regarding affordability programs they are potentially eligible for. Affordability conversations can naturally branch off of the standard Access workflows (as managed in hub CRM systems) of benefits verification, prior authorization, and therapy fulfillment.
Executing on a highly personalized, patient-centric affordability effort can have tremendous impact on first fill and adherence rates. In one recent example, an Access team at a partial-onset seizure medication provided every patient with a conversational digital assistant throughout the first fill process.
The team saw that patients interacting consistently with the digital assistant filled at a 10% higher rate compared to patients not interacting with the digital assistant.

They also spent 18% more time on therapy.
 This case study provides a glimpse into what the future of affordability-focused engagement might look like.
This case study provides a glimpse into what the future of affordability-focused engagement might look like.
Just-in-time, low friction conversations via mobile messaging can enable pharmaceutical companies to provide clear next steps, manage enrollment, and gather real-world comprehension and adherence insights from patients. Executing on this type of engagement approach can create a seismic shift in patient awareness and participation in affordability programs, improving outcomes, and instilling trust with patients.